
Highly pathogenic avian influenza virus ‚Äď particularly the ‚Äď has transformed the global disease landscape over recent years.
What was once largely a poultry disease causing occasional severe illness in humans is now a , affecting wild birds, mammals and increasingly, entire ecosystems.
Despite more than five years without incursion, H5N1 2.3.4.4b is edging closer to New Zealand, raising questions about how long our isolation will hold.
Importantly, spillover events ‚Äď when a virus jumps between species ‚Äď have become more common, with large outbreaks reported among poultry and in North America.
Human infections remain rare and are mostly linked to close contact with infected animals. But every spillover event gives the virus another chance to evolve, even without sustained human-to-human transmission.
Why hasn’t it reached Oceania yet?
The current H5N1 strain is unprecedented in both scale and scope.
Its host range now spans hundreds of bird species and an increasing number of mammals, including . This expansion reflects increased exposure and the virus’s ability to adapt to new hosts.
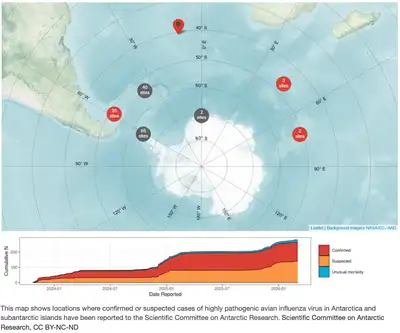
Geographically, the virus has spread across Europe, Asia, Africa, the Americas and, more recently, the Antarctic and sub-Antarctic regions, with .
Yet Oceania has so far remained free of H5N1 2.3.4.4b. This is largely due to geography and bird migration patterns. Many migratory birds that carry H5N1 move along northern hemisphere flyways and do not typically reach New Zealand.
However, New Zealand hosts large numbers of migratory birds via the East Asian-Australasian Flyway, including shorebirds that can carry avian influenza viruses, although they are considered a lower-risk reservoir.
There is also the possibility of a ‚Äúgrowing our own‚ÄĚ problem. Low pathogenic influenza viruses circulate naturally in wild birds in New Zealand. Under the right conditions, particularly in poultry, these can evolve into highly pathogenic forms.
This risk is not hypothetical. A recent poultry outbreak in New Zealand caused by likely arose from local low pathogenic viruses in wild birds.
While distinct from H5N1 incursion, the consequences could be similarly devastating. Although this outbreak was contained to a single farm, it underscores how quickly events could escalate if early transmission is not controlled, stretching resources and prolonging response efforts.
Given the , transmission to could challenge our key primary industries. This has happened independently on .
Risks to New Zealand’s wildlife
New Zealand’s wildlife is to H5N1. Many native species are already under pressure from habitat loss, climate change and introduced predators.
The arrival of a highly pathogenic avian influenza virus would add a new and potentially severe threat, particularly for small or isolated populations.
Taonga species, including seabirds, shorebirds and endemic waterfowl, may be especially at risk. New Zealand wildlife has had little to no exposure to these viruses, and therefore limited opportunity to develop any resilience.
Species that breed in dense colonies, such as tńętńę, albatross and penguins, could be particularly vulnerable to rapid spread and mass mortality events.
The risks are not confined to birds. The impact of H5N1 2.3.4.4b on marine mammals has been severe. This is well illustrated by the plight of elephant seals.
Recent deaths of in critical breeding are concerning, but the impact of the virus on threatens the in South America and the sub-Antarctic.
Transmission between marine mammals may be important, highlighting risks to other vulnerable populations.
Southern elephant seals and , share similar habitats, including . An outbreak of H5N1 in breeding colonies in the sub-Antarctic and populations in Otago and Rakiura could set back recent conservation efforts.
Why vigilance is NZ’s best protection
Vaccination has been explored internationally, particularly in poultry, as a way to reduce disease burden and transmission.
In New Zealand, have been implemented for a small number of taonga species held in captivity.
However, vaccination is not currently a practical or effective option for free-ranging wildlife populations. As such, prevention and early detection remain the primary tools available.
Wildlife surveillance has increased in recent years, including targeted sampling of wild birds and environmental monitoring at . To date, there is no evidence of H5N1 2.3.4.4b in New Zealand.
However, surveillance systems are limited in their ability to detect rare or early incursions. Ongoing vigilance, including public reporting of sick or dead wildlife, will be critical for early detection and response.
Ultimately, New Zealand’s strongest defence remains time and preparedness
The country’s geographic isolation has bought it a window to strengthen surveillance, improve coordination across wildlife and agricultural sectors and . But that window will not remain open indefinitely.
The global trajectory of H5N1 suggests that incursion is a matter of when, not if.
Ensuring rapid detection, strong biosecurity measures and the capacity to scale interventions will be critical to limiting impacts on Aotearoa’s wildlife, primary industries and ecosystems.
Distinguished Professor Nigel French is an infectious disease epidemiologist and public health expert. He teaches within the School of Veterinary Science at Te Kunenga ki PŇęrehuroa √Ř∂Ļ ”∆Ķ.
This article was first published by , and was co-authored with Professor Jemma Geoghegan, ŇĆtńĀkou Whakaihu Waka University of Otago.